Upper Valley Sees Health Concerns in Broad Terms
 Over the past decade, public health and health care professionals have recognized that health care services only account for a small portion (10 to 20%) of a person’s health status. The rest of one’s health status can be attributed to social and economic factors, the physical environment, and health behaviors. These drivers of health are known as the Social Determinants of Health.
Over the past decade, public health and health care professionals have recognized that health care services only account for a small portion (10 to 20%) of a person’s health status. The rest of one’s health status can be attributed to social and economic factors, the physical environment, and health behaviors. These drivers of health are known as the Social Determinants of Health.
Improving community health is at the core of the mission of the Public Health Council of the Upper Valley. Most of our partners share this goal, but contribute in different ways to reaching that goal. Some partners are health care providers, some provide treatment for substance use disorders or mental illnesses, others support people in our communities who struggle with various social determinants of health.
Every three years, the Public Health Council works with area hospitals to conduct a routine community health needs assessment. These assessments form the basis for updating priorities and give us insight into what concerns community members. Over the course of 2021, the Public Health Council supported data collection efforts led by Dartmouth-Hitchcock, Alice Peck Day Memorial Hospital, VNHVNA, and Mount Ascutney Hospital and Health Center. Each health care organization uses the results to create Community Health Improvement Plans for their organizations. The Public Health Council will work with many partners across the region to generate a Community Health Improvement plan that reflects to great work ongoing in our region, leverage our strengths, and challenge our partners to find and fill gaps together.
Community Health Needs Assessments Available Online
To review the most recent Community Health Needs Assessments and related documents by hospital service area or organization:
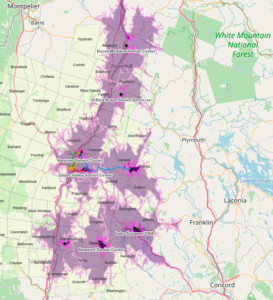
The Upper Valley Community Health Needs Assessment generated for the Dartmouth-Hitchcock Alice Peck Day primary hospital service areas covers 19 municipalities in Vermont and New Hampshire, with a total resident population of 69,612 people. Data came from over 1,600 survey responses from community residents; a direct email survey of key stakeholders and community leaders; a set of community discussion groups; and a review of available demographics and health status indicators. The New Hampshire Community Health Institute conducted the survey, data analysis, and report generation. Throughout the process, they were careful to focus on vulnerable and disproportionately served populations in the region.
Taking It Back to the Community
Beginning in February 2022, the Public Health Council worked with partners at Dartmouth-Hitchcock, Alice Peck Day Memorial Hospital, Visiting Nurse and Hospice for VT to share the results with members of our communities. We co-hosted two virtual Community Health Improvement Summits open to all community residents. Our health care partners reviewed the priorities emerging from the recent results. Participants shared their thoughts about what the results tell us, what opportunities we have to address them, and what strategies we might help.
The top six priorities emerging from the results are:
- Availability of Mental Health Services
- Cost of Health Care Services (Including Dental Care)
- Access to Affordable and Nutritious Food
- Substance Misuse Prevention and Treatment
- Child Wellbeing
- Social Determinants of Health (Especially Housing)
The input we received from the two summits, attended by over 125 people, can be found in a report dated April 13, 2022: FY22 CHNA Summit Theme Report.
Recordings of the virtual Summits are available online:
Recording Link: UV Community Health Improvement Summit #1
Date: Feb 23, 2022 08:42 AM Eastern Time (US and Canada)
Recording Link: UV Community Health Improvement Summit #2
Date: Mar 2, 2022 05:14 PM Eastern Time (US and Canada)
Shaping a Plan for Our Communities
For the remainder of 2022, the Public Health Council and partners will work together to create a Community Health Improvement Plan. The Plan will address the priorities by laying out what success would look like and how we can achieve it.
For more information about the community health improvement planning process or ways you can participate, please contact Alice Ely at the Public Health Council.